
The typical age groups that suffer from atopic dermatitis include mainly children and infants, but also adults. In Germany, around 2 million children and 2.5 million adults are affected by atopic dermatitis.
Often, atopic dermatitis first appears in infancy and childhood and typically recurs in episodes. Symptoms can alleviate or even disappear with advancing age.
Patients have to struggle primarily with the symptoms of dry and scaly skin, which is accompanied by eczema (skin rashes). The affected areas are red, inflamed and, if they persist for a long time, wrinkled. In addition, sometimes pustules, crusts and blisters can develop, which often weep. This is usually accompanied by severe itching, which is also particularly pronounced at night and can lead to fatigue and difficulty concentrating in those affected due to sleep disturbance. However, the cycle is aggravated by scratching and the symptoms are thus intensified. The recurring inflammations can lead to a thickening of the respective affected skin area (technical term: lichenification) in the long term and mostly occur on the wrists as well as the crooks of the arms and the backs of the knees.
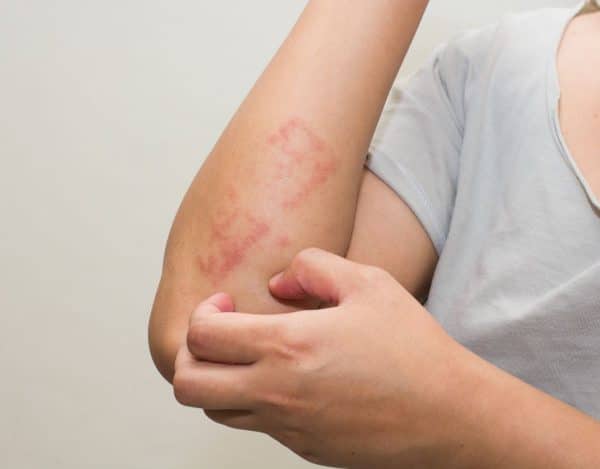
In the following, you will find common body parts where symptoms occur in the different age groups.
Face, especially cheeks and head
Arms and legs
Bend
Excursus: Cradle cap is an inflammatory rash on the scalp and face of infants. It often appears after the third month of life and heals after some time. It may be associated with the onset of atopic eczema.
Important: However, cradle cap alone is not directly a sign of atopic dermatitis.
Face, especially forehead, eyes and mouth
Neck and nape of the neck
Wrists
Hands
Bending wrinkles
Scalp
Eyelids
Earlobes and lip area
Neck and face
Hands and feet
Genital area
Of course, the body areas cannot be generalized and differ from person to person. In children and adolescents it is more often the case that atopic dermatitis is often likely to “grow out” over time. In adults on the other hand it often persists and recurs in a certain body region, e.g. through eyelid eczema, head eczema, hand/foot eczema or genital eczema.
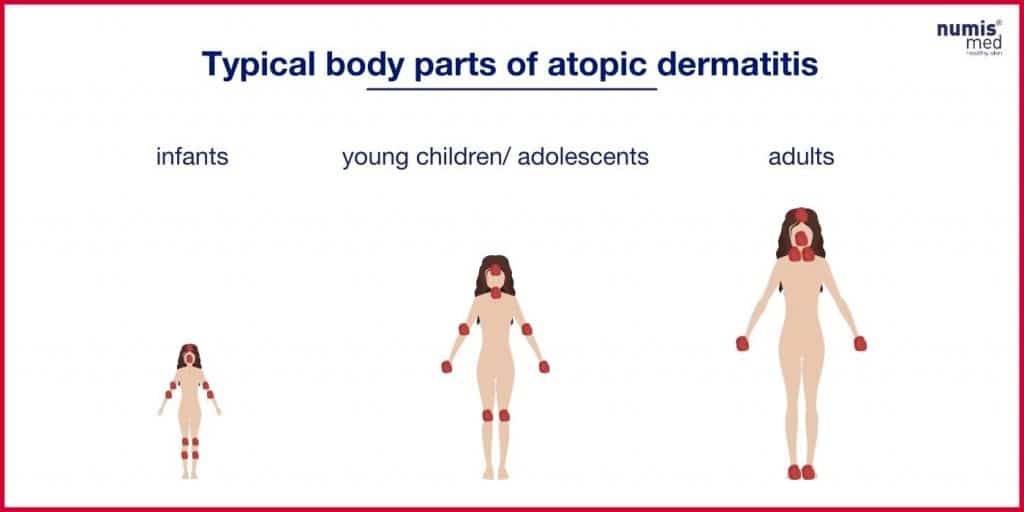
Since the independent differentiation from dry skin as well as from other skin diseases is difficult, finally only a physician can make a specific statement about whether skin changes are atopic dermatitis.
Nevertheless, there are signs that speak for atopic dermatitis:
Other atopic diseases (asthma, hay fever, allergies) in oneself or within the family
Relatives with atopic dermatitis
Recurring eczema, especially episodic
atopic eczema manifestations at an early age
Characteristic expression and distribution of eczema for age
Itching
The skin turns white after scratching (usually it turns reddish as soon as you scratch) – this is the so-called white dermographism.
Since a complete cure of atopic dermatitis in the strict sense is not yet given, the goal of treatment or therapy is to alleviate the symptoms of those affected as far as possible and to stabilize/extend the symptom-free interval as much as possible. On the one hand, the therapy consists of basic care, which should ideally be carried out every day and also always directly after showering/bathing. Creams and lotions containing urea and glycerine play the main role here. In addition to the daily application, it is also important to use a sufficient amount.
Besides the basic care, treatment of inflammatory relapses and also the maintenance therapies for relapse prophylaxis are necessary.
Within the conventional medical approach, the following therapies are applied:
Basic care (creams/ointments with moisturizing factors such as glycerine and/or urea).
Avoidance of triggers
Prevention and treatment of infections
Anti-inflammatory external therapies (e.g. calcineurin inhibitors, modern cortisone creams/ointments with high therapeutic index, i.e. few side effects with very good efficacy)
Light therapies (Psoralene bath plus UVA for hands/feet for hand-foot eczema, salt bath plus narrowband UVB)
Internal therapy with immunosuppressants (Ciclosporin A) – very rarely used now because of side effects
Modern immunomodulating therapies in the form of subcutaneous injections/pens (Dupilumab, Tralokinumab)
Modern oral therapies in tablet form (JAK inhibitors).
In case of allergies: Allergen avoidance and if this is not sufficient: hyposensitization.
As an alternative or supplement to conventional medicine, many patients familiarize themselves with complementary medicine. These include, for example, homeopathy or acupuncture. Although these approaches have not yet been scientifically proven, they can also have positive effects on an individual basis.
Basically, it is above all important for those affected to get to know themselves well or to manage themselves well. There is the possibility to participate in so-called atopic dermatitis training courses, in which one can learn an optimal handling of the disease. In addition, it makes sense to take care not only of the physical concerns, but also of the psychological factors and to find an individual way to deal with them in a targeted manner, even in more difficult phases.

Due to the everyday wearing of a protective mask, our facial skin faces great challenges. As a result, irritation, impurities and dry patches can occur on the face, especially in sensitive skin. But even normal skin often shows irritations and skin irritations due to the increased use of a mouthguard, which can eventually lead to dry skin under the mask.
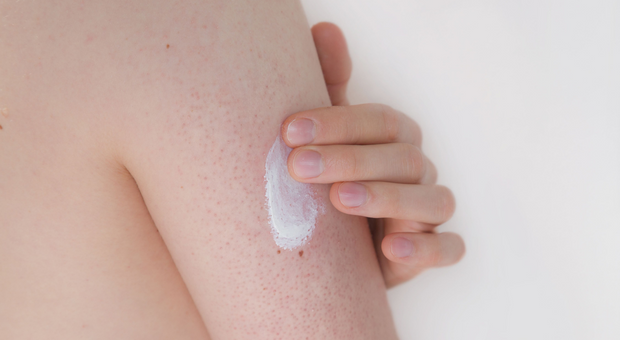
Keratosis Pilaris, Lichen Pilaris or Follicular Keratosis, colloquially known as chicken skin, has many names. But what exactly is the cause of this skin condition and We reveal what symptoms are and how to care for and treat rubbing iron skin.
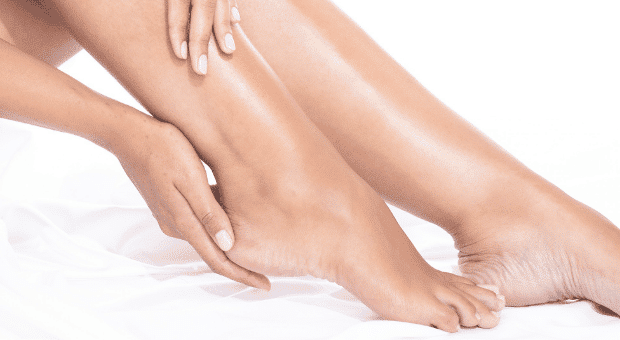
Struggling with dryness and cracking on your heels? Here you can learn more about the prevention and treatment of chapped or dry feet.

In the following article you will learn more about the causes of dry elbows and how you can best prevent them. Causes can include hormones, lifestyle, dry air and clothing material.

Limy water can lead to dry skin and skin diseases. Learn more about the influence of water hardness on our skin here.

The skin protects the body from external influences. But the skin itself also needs protection: the skin's microbiome is responsible for this.